| I
am Ilse Montocchio, the
mother of 4 children. Our
third child, Gerard, is
brain-injured.
We have been doing an
Intensive Treatment
Program from the
Institutes for the
Achievement of Human
Potential (IAHP) for 1
year and 10 months. |
 Gerard at 4 yrs
Gerard at 4 yrs
|
| GERARD
MONTOCCHIO
Gerard
was born on 10 October
1995 in Vienna, Austria.
He weighed 5 kg and looked
completely healthy. He did
not drink well, and became
more and more lethargic.
When he was two days old,
he was taken to the
emergency unit of the Pediatric
Clinic of the
General Hospital. At this
time, he had only 20%
Oxygen in his blood. He
was diagnosed with a
Transposition of the Major
Arteries, a serious heart
defect where the Pulmonary
Artery and Aorta are
switched. He was put in an
artificial coma and
artificially respirated.
He was immediately
operated upon (Rashkind-Manoever)
, and had a rough time for
quite a while, including a
period on a heart-lung
machine, kidney failure
and dialysis, heart
failure briefly, and then
at the age of 17 days, on
the 27 of October, he had
an arterial Switch
Operation, a 5-hour
operation where the
Pulmonary Artery and Aorta
are severed and sewn on in
the correct position. He
then developed
Hydrocephalus (water on
the brain), so on the 23rd
of November he had a
Ventricle Peritoneum
Shunt-implantation with a
Low-Pressure-Valve, to
ensure that the brain
fluid can be drained off
properly. He had one
seizure, and was put on
Phenobarbital. A Computer
Tomography showed that he
had extensive hypoxic
brain damage, with a
triangular-shaped lesion
in the occipital region.
Visually Evoked Potential
and Auditory Evoked
Potential Tests indicated
that both his vision and
hearing were
neurologically impaired.
After 2,5 months, he was
released from hospital,
still being tube-fed
through the nose, and
hardly able to move his
limbs. His general
progress since then, was
very slow but steady. He
never had any serious
setbacks, and is very
healthy.
Therapy
until April 2000, aged
4,5:
Logopaedic
therapy: Daily for the
last 3 weeks of hospital
stay, then one hour weekly
for next 1,5 years.
Physiotherapy:
Bobarth-therapy daily for
the last month of hospital
stay, then Vojta-therapy
one hour weekly until age
4,5. I did 2 sessions of
Vojta-therapy (15 minutes
each session) with Gerard
on a daily basis.
Cranio-sacral
therapy: One hour weekly
from age 4 months until
age 4,5 years
Occupational
therapy: 1,5 hours weekly
until aged 4.
Hyperbaric
oxygen therapy: 20
sessions in January 2000,
aged 4 years and 2 months.
Development
until April 2000:
Mobility:
When he was one year old,
he learned to turn from
his back onto his side. By
21 months, he had learnt
to roll over from both
back and tummy, and could
log-roll as a means of
transport. Just before his
4th birthday, he learnt to
move forward by pulling
himself along on his
belly. In April 2000 he
could crawl a maximum of
10 meters per day, in
half-a-meter stretches at
a time.
Vision:
Over the years, his severe
nystagmus had improved a
lot, but he still had
alternating divergent
strabismus. He was
functionally blind, as he
could only see outlines
against a strong light,
and could occasionally
follow moving objects. He
had a weak, inconsistent
light reflex.
Hearing:
He was almost deaf, could
only hear over 90 Decibels
(as loud as standing right
next to a big passenger
airplane taking off!)
Tactility:
He could not feel any
pain, hot or cold, but
enjoyed it when we tickled
him in his neck.
Manual
dexterity: By age one he
could grasp objects with
both hands, using the
thumb and all four
fingers. He had not
progressed to a pincer
grip.
Muscle
tone: A mixture of
hypotonic and hypertonic.
He tended to arch his neck
back-wards. His truncal
tone was hypotonic, and he
had difficulty holding his
torso upright. Over the
years, his legs had become
very rigid (spastic).
Both hips were dislocated,
his legs scissored, both
feet turned outwards and
downwards. The hamstring
tendons in his legs were
shortened, his legs were
permanently bent and could
not be straightened. His
hands and arms were
becoming increasingly
rigid.
General
Health: Excellent, but he
had not put on any weight
in the last 1,5 years. He
had problems with reflux
(vomiting) 5 times a month
on average.
After
consulting with our
homeopath, we slowly
weaned him off
Phenobarbital. When he was
one year old, he was
detoxified, and he has not
had any seizures since.
IAHP:
In
February 2000, a friend
gave me the book
"What to do about
your brain-injured
child"
by Glenn Doman, and both
my husband and I decided
immediately that we had to
try this therapy program.
In April 2000, we attended
the 5-day course
"What to do about
your brain-injured
child" in
Philadelphia. There we
learnt how to evaluate and
design a home program for
Gerard. In May we started
an intensive therapy
program, working with
Gerard 8 hours per day, 7
days a week. After 3
months, we sent in a Home
Program
Consultation,
after which a staff member
called us for an hour-long
consultation, suggesting
changes to his program
based on the progress that
he had made. In October
2000, we went to
Philadelphia with Gerard
for his first 2-day
aspirant appointment. He
was evaluated by the
staff, and they designed
and taught us a new
program based on the
progress that he had
made.
We
now go to Philadelphia
every 6 months for a 5-day
visit, which includes
evaluation, 2 days of
lectures, and a new
program that is taught to
us.
My
e-mail address: poppie@aon.at |
|  |
|
 Gerard at 4 months
Gerard at 4 months
|
|
IAHP
THERAPY:
The most important principle is that
the brain grows by use brain growth and development can
be slowed down or stopped by brain injury, BUT it can also
be speeded up (plasticity of the brain). Everything that we
learn, is learnt through the five sensory pathways into the
brain seeing, hearing, feeling, taste and smell. Brain
injury creates a "barrier" between the environment and
the brain, and a normal stimulus or input (enough for a well
child to develop in all facets) will not get through to an
injured brain.
Therefore the frequency (how often
during the day you do each activity), intensity (how bright
the light in visual stimulus, how loud the sound in auditory
stimulus, how far does the child move in mobility, etc) and
duration (the length of time you do each activity) has to be
high enough, otherwise the message will not arrive in the
brain. With 60 years of experience in treating brain injured
children, the Institutes know exactly at what intensity,
frequency and duration each part of the program has to be
done, for the children to progress. The brain injured child's
capabilities are evaluated in the
three most important input pathways (seeing, hearing and
feeling) and the output pathways (mobility, language and
manual competence). (See the
Institutes developmental Profile at http://www.iahp.org/developmental_profile/index.html
)
A program is then designed and taught
to the parents which helps the child develop
from one stage to another in each pathway through activities
which reinforce the level that the
child is at, and stimulate the next level.
Excellent nutrition, eliminating
harmful chemicals (purifying water and air),
respiratory programs to increase the oxygen supply, and
intellectual programs (reading,
maths and intelligence bits) are vital ingredients of the Institutes¹
programs.
The Institutes believe that the
parents are the answer parents know their kids the best
and love them unconditionally and are willing and capable of
working with their kids for many hours daily until their
child reaches its true potential.
Gerard's program has included:
I will only describe Gerard¹s program
in general terms, because each program has to be taught to
the parents by the IAHP staff. The program changes as the
child develops.
Vision:
a) Stimulating the light reflex with a
flash light
b) To create outline perception:
Environment around him with checkerboard wall; showing him
black and white outline bits
c) To learn to see detail: Colorful
shapes on checkerboard; detail bits with color
Hearing:
a) Banging two wooden blocks together
b) Other loud noises, like banging
pots and pans, sirens, whistles, etc.
c) Environmental sounds, for example
bells, clapping hands, telephone ringing, musical
instruments
d) Transient Electronic Auditory
Stimulation based on the work of Guy Bérard, TEAS are
CD¹s with music on it, interspersed with powerful,
short-duration, random, high-frequency pulses.
Tactility:
a) Contrasting stimulation of hot and
cold; stimulating with sharp fingernails
b) Contrasting stimulation of rough
and smooth
Mobility:
a) Cross-Patterning: Three adults move
the child¹s limbs and head through
the movements of crawling or creeping.
The child lies on his tummy on a table. This is not physical
exercise for the child, it is a sensory experience, telling
the child¹s brain "This is how it feels to creep"
b) The Floor as a Way of Life:
Spending every available moment on the floor on his tummy.
c) Belly-crawling on a smooth surface
wearing an anti-roll device. Log-rolling is a dead-end in
mobility development, it doesn¹t lead to the next stage of
mobility, creeping the anti-roll device prevents the
child from rolling over. He learns that if he wants to move,
he must crawl.
d) Crawling on carpet.
e) Medullary Reflex Program rolling
down an incline.
f) Body Weight Suspension Program
hanging upside down. Gravity helps to stretch his shortened
tendons, improve scoliosis and hip luxation.
g) Assisted creeping with an anti-sit
device on Two adults move his arms and legs in
cross-pattern creeping; the anti-sit device supports his
legs.
h) Creeping on all fours in the
Gravity-Assisted Environment: The child is given the
opportunity to FEEL what it feels like to move using his own
brain and balance areas of his brain. He wears a harness, to
which are fastened bungee cords that come down from a track
attached to the ceiling. He is put in the quad position with
four cords attached to his shoulders and hips.
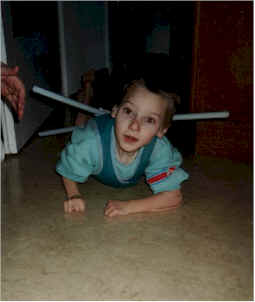
Gerard wearing his anti-roll device
Respiratory Programs:
a) Reflex mask
b) Positive Respiratory Machine
c) Oxygen Enrichment Program
NB: The respiratory programs can and
should only be done when they are prescribed by IAHP, as
there are some contra-indications.
Nutrition:
No sugar in any form; no milk
products; very little salt, liquid balance; a healthy
balance between proteins, carbohydrates and fats in every
meal; vitamin and mineral supplements. For the last 6 months
all the foods that he is allergic to has been taken out of
his diet.
Update Reports
Progress since starting the IAHP
program in May 2000
Mobility: After 8 months on the
program, he reached his belly-crawling goal of 300 metres
per day on the smooth surface. He then started crawling on
the carpet (which is a lot more strenuous, as there is more
friction), and reached his carpet crawling goal of 300
meters per day on 2 December 2001, 19 months after starting
the program. He can now push himself up into a quad position
on all fours, and hold it for 4 minutes. He is well on his
way to learning to creep on all fours. His strength, balance
and stamina has increased vastly. He can crawl 25 meters in
one go. I am 100% convinced that he will learn to walk with
time, based on the many children that I have seen at IAHP
who have made the same mobility progress as Gerard.
Vision: After 2 months on the program,
Gerard could track objects accurately and fast. After
another 2 months, he started seeing detail, which means that
he could see facial expressions and mimic them. He can now
see tiny objects on the floor (as small as a piece of
fluff), crawl to them and pick them up. His nystagmus has
completely disappeared. His strabismus has improved he is
alternating much faster between his eyes. He crawls to
stairs, sees that they are going down, and will stop before
the stairs.
Hearing: This is the area of least
progress. He reacts much more often to sounds (turns his
head towards the sound), but does not do this all the time.
Tactility: After 3 months on the
program, he reacted properly to pain, hot and cold, pulling
away from the stimulation. He can now feel and react to
gentle touch all over his body.
Speech: The volume of his babbling has
increased 10 times. He hardly ever cried, now he lets us
know when he is unhappy or has hurt himself! He is making
many more sounds much more frequently, but his speech
development is dependent on his hearing. He will have to
hear better before he will be able to improve his speech.
Manual competence: He has not yet
developed a pincer grip (grabbing objects between thumb and
index finger), but he can grab objects much faster, hold
them for a long time, deliberately let go of objects, bang
two sticks together.
Weight: In the first year of program,
he put on 1,5 kg, and then stayed at this weight, despite a
high calorie diet of 1 500 calories per day. We had every
conceivable conventional test done (stool, allergy, thyroid,
growth hormone tests), but every test came back negative. In
October 2001, the nutritionist at IAHP did a kinesiology
muscle test, and found several foods and environmental
substances that he was allergic too. From the moment that we
cut out the foods that he was allergic too, he started
eating really well, had no more reflux, and put on 1 kg in
one month!
General: Within one month of starting
the program, his feet were almost straight and had a lot
more tone. The rigidity in his hands and arms have improved
a lot, his left hand (the hand he uses the most) is
beautifully loose. The rigidity in his hips and legs have
improved tremendously. His legs are now nearly straight, his
legs can be opened to an angle of 90° (before program
30°). He has finally realized that he has legs and that
they can be used! He can now swallow liquids without
choking. Feeding him is a pleasure, previously half the food
fell out of his mouth. He is now using his tongue to move
the food to the back of his throat. He knows the members of
his family he gets very upset and starts crying when one
of us leaves the room and leaves him alone. His legs used to
look like sticks, he had no noticeable muscles now he was
super-duper thigh, tummy, back and arm muscles. When we pick
him up, he grabs us round the neck to give us a hug.
He can be held upright just by holding
him under his bottom previously he would have flopped
backwards immediately. According to IAHP¹s evaluation in
October 2001, he has progressed 9 times faster in the 1,5
years that he has been on the program, compared to the
entire 4,5 years before he started the program.
Why has he progressed so much faster
with the intensive IAHP program?:
First of all, the other therapies were
not intensive enough in terms of time to make a real
difference for a profoundly brain-injured child like Gerard.
Secondly, each therapy program that we
pursued addressed only one specific area of his development.
For example, Bobarth-therapy is a neurologically-based
physiotherapy, but because he did not spend enough time on
the floor on his tummy, his mobility development was much
too slow.
Without solving the problem of
increasing spasticity, his mobility development would have
slowed down even more, and he would probably have regressed.
The Institutes' program addresses
every area of development in a structured way. Everything is
interdependent if the child can¹t see well enough, he is
not motivated to move. If he can¹t feel where his leg is,
he can't move.
If his breathing is inadequate, he has
no stamina to move. If his nutrition is bad, his brain and
body is not getting the nutrients it needs to function
properly. If he is too thin, he has no stamina to move
enough to be able to get to the next stage in mobility
development, etc. On the other hand, every bit of progress
in any area has a positive influence on the other areas.
I have been amazed at his progress in
the last year and 10 months, and look forward to his further
development he has not nearly reached his true potential.
Contacts:
The Institutes for the Achievement of
Human Potential: http://www.iahp.org/
|
|

